Psoriasis treatments, triggers and facts
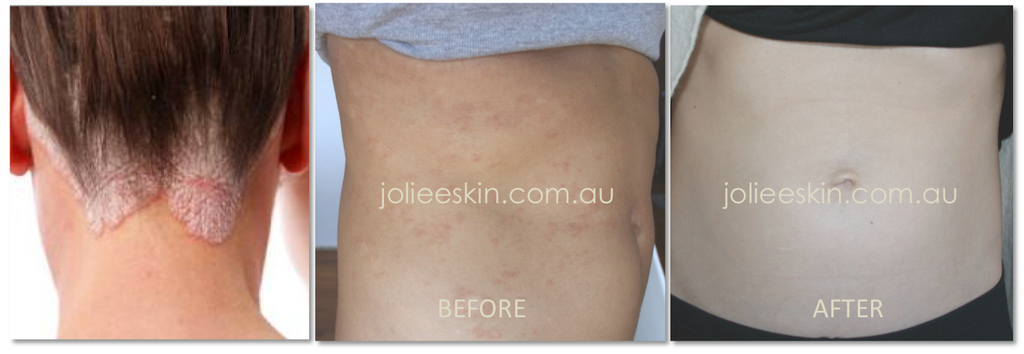
Psoriasis (pronounced "sore-EYE-ah-sis") is an inflammatory skin disease where the skin cells grow too quickly resulting in white, silvery or red, thick patches. In healthy skin, the skin cells mature in approximately four weeks but with psoriasis they can mature in as little as three to four days, resulting in flaky build-up. It’s as if the skin is desperate to expel something irritating from within so it prematurely forces skin cells to the surface.
Psoriasis can be itchy and occasionally painful but it’s not contagious.
Psoriasis Facts
Psoriasis can range from mild to moderate to very severe. The psoriasis rash can occur on any part of the body but it most commonly occurs on the scalp, face, elbows, knees and torso. Psoriasis can also develop under/on the nails, palms, genitals and on the soles of your feet.
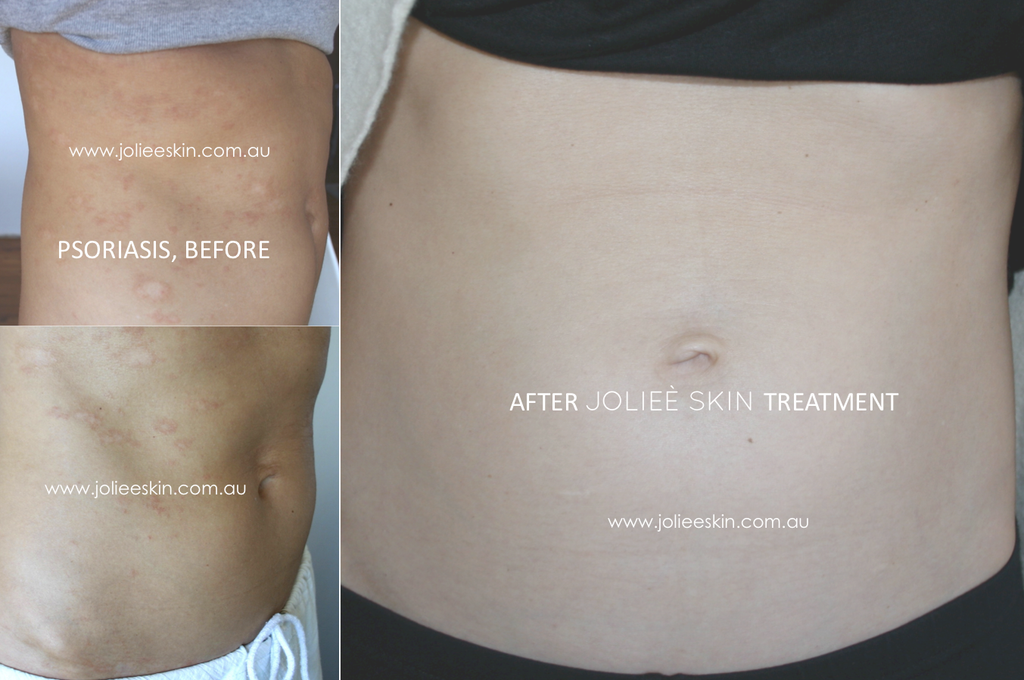
There is a treatment plan plus before and after photos at the end of this article.
Common psoriasis symptoms:
- Silvery or white scales
- Red rash
- Itchy and tender skin
- Flaking, dry skin
- Patches can join together and cover large areas (e.g. back)
- Joints can be swollen and painful (known as psoriatic arthritis)
- Fingernails/toenails change colour, pit, and separate from the nail bed
- Dead skin build-up under nails
How is psoriasis diagnosed?
A doctor, dermatologist or other health care provider usually examines the affected skin and determines if it is psoriasis. A skin sample may also be sent to a lab for testing, if necessary.
Types of psoriasis:
- Plaque psoriasis (most common type), also known as discoid psoriasis. Symptoms may include patches of red, raised skin on the trunk, arms, legs, knees, elbows, genitals, and/or scalp. Nails may thicken, become pitted, and separate from the nail beds.
- Guttate [GUH-tate] psoriasis is characterised by small dot-like lesions. This type of psoriasis affects mostly children. A sore throat usually precedes the onset of this type of psoriasis.
- Pustular psoriasis has weeping lesions and extensive scaling. It may occur on the palms, soles and other small areas or over the whole body.
- Inverse psoriasis is characterised by severe inflammation.
- Erythrodermic [eh-REETH-ro-der-mik] psoriasis has extensive shedding and redness of the skin.
- Psoriatic arthritis presents with fatigue, tenderness, pain and swelling over tendons; swollen fingers and toes; stiffness and pain in one or more joints; reduced range of motion; morning stiffness and lethargy; red eyes and nail changes (nail separates from bed, pitting and fungal infections may occur). In 85% of patients, psoriasis precedes the joint disease so tell your doctor if you have psoriasis plus aches and pains.
Psoriasis can also appear when the skin has been injured, for example, from vaccinations, sunburns and scratches. This is called the Koebner [KEB-ner] phenomenon. The Koebner response can be treated if it is diagnosed early. The symptoms of psoriasis may resemble other dermatologic conditions so consult a physician for a formal diagnosis, before booking a consultation with Karen.
Q: “What age does psoriasis usually appear?”
Psoriasis commonly develops between the ages of fifteen and 40 but it can occur at any age.
More than 75% of psoriasis cases occur before the age of 40.
Approximately 10% to 15% of people with psoriasis have it earlier than age 10.
Some infants have psoriasis, although this is very rare.
Psoriasis and genetics
People with psoriasis usually have an underlying genetic tendency that makes them susceptible to getting the condition. Scientists believe about 10% of the population have this genetic tendency. However, only 2-3% of the population develops psoriasis as it can lie dormant for many years and may never appear unless it’s awoken by some sort of ‘trigger.’
Psoriasis triggers
Psoriasis can be triggered or aggravated by the following:
- high chemical exposure (this is common but many people don’t know they’ve been exposed)
- cigarette smoke, smoking and passive exposure
- injury
- throat infection/poor health
- drugs/medications
- physical or emotional stress
- alcohol
- anxiety and worry
- chemical cleaning products
- flea/cockroach ‘bombs’
- living on a farm near crop spraying (chemical exposure)
- trauma to the skin (scratch/surgery)
- vitamin and mineral deficiencies (this is common)
- cold climates
- poor digestion, bowel toxemia
- impaired liver function
- eating excess meats/saturated fats
- candida albicans
Smoking and psoriasis – the common trigger
A scientific study found that the more cigarettes you smoke and the longer the duration as a smoker, the more severe your psoriasis becomes.
Working out what caused your psoriasis
If your psoriasis appeared during adulthood or in your later childhood years then it’s a good idea to try to figure out what may have triggered it. The following activity is from The Healthy Skin Diet:
Questionnaire: When did your psoriasis first appear?
Think back to when your psoriasis first appeared — what was going on in your life at the time? For example,
- Were you exposed to a new chemical or food?
- Did you move house?
- Did you renovate your house or put in new carpets?
- Was your home or office sprayed with pesticides or were the carpets chemically cleaned?
- Were you under great financial or personal pressure?
- Were you feeling rundown with a virus or throat infection? Earache, bronchitis, tonsillitis or a respiratory infection?
- Were you prescribed a new drug or were you using pain-killers or another kind of medication?
- Were you self-medicating with alcohol or cigarettes?
It’s important to work out what may have switched on your ‘psoriasis’ gene so you can see if you’re still being exposed to the problem. For example, if you figure that stress triggered your psoriasis then you can make sure you include relaxation techniques in your healthy skin program. If your trigger was a throat infection, then you can support your immune system with relaxation and supplements, foods such as garlic and the Anti-ageing Broth (Healthy Skin Diet or Eczema Diet recipes).
Medications that trigger psoriasis
Some medications are associated with triggering psoriasis, including:
- Lithium: aggravates psoriasis in about half of those with psoriasis who take it.
- Antimalarials: Plaquenil, Quinacrine, chloroquine and hydroxychloroquine may cause a flare of psoriasis, usually 2 to 3 weeks after the drug is taken. Hydroxychloroquine has the lowest incidence of side effects.
- Inderal: worsens psoriasis in about 25 to 30% of patients with psoriasis who take it.
- Quinidine: This heart medication has been reported to worsen some cases of psoriasis.
- Indomethacin: can worsen some cases of psoriasis. Other anti-inflammatories usually can be substituted.
If you suspect your skin problem may have been triggered by a prescribed drug (and you’re still taking it) then speak to your GP about possible alternatives (FYI: don’t stop taking the drug without speaking to your doctor first).
Q: "I have psoriasis, it’s extremely uncomfortable and I’m shedding skin everywhere. What can I do to get some relief and reduce flaking?"
Water, oil and light therapy
A common therapy for treating psoriasis is sunlight therapy and when you combine it with this Healthy Skin Diet treatment plan (with water and oiled skin) you get some relief. Water, oil and light therapy (I like to call it WOL therapy) is natural, it doesn’t have the negative side effects that corticosteroids have and it’s practically free. I recommend using WOL therapy in conjunction with a healthy diet and the psoriasis supplement (requires a prescription) for long-term results.
Psoriasis Research
An eight-week study published in the International Journal of Hypothermia found that warm bath treatments were also very effective in healing flaky lesions in psoriasis patients. Seven people were asked to take very warm baths twice a week and three of them showed a rapid improvement in symptoms; the other four were told to increase bathing to every second day and three out of the four had improved symptoms. Only one person’s lesions did not improve with bath therapy and coincidentally he was the only person in the study who was also using prescribed drug therapy. So WOL therapy may not work in conjunction with conventional psoriasis medications but please speak to your doctor first before discontinuing your prescribed drugs.
Psoriasis and vitamin D research
Another study found that people with severe psoriasis have decreased blood levels of vitamin D, compared with clear-skinned people and people with only mild psoriasis. You can obtain a daily dose of vitamin D by simply going out in the sun, because UV rays from sunlight trigger vitamin D production in the skin. (Being covered from head to toe with sunscreen can block vitamin D production so skip the heavy-duty sunscreen during WOL therapy — but use sunscreen if you are spending more than fifteen minutes in the sun.) Keep sunshine therapy to a healthy minimum, which is about ten to fifteen minutes a day.
Try this psoriasis treatment plan from The Healthy Skin Diet (this is my book so I have permission to publish the info online for you…). As I mentioned in the book, I had psoriasis over half of my body and this was a part of my treatment plan that got rid of it (I also used a psoriasis supplement).
WOL therapy step by step
Begin by wetting your skin with warm water — either by having a very warm bath, a shower or by splashing yourself with water. Keep in mind that it’s best to allow the water to soak into the skin for a few minutes. Bathing is also a safe and effective way to gently remove some of the excess skin.
Pat your skin semi-dry, leaving some moisture on the skin, then rub in tiny (must be tiny!) amounts of natural pawpaw ointment. When applying the ointment remember that the less you use the better it works. Gently rub in the ointment until it’s completely absorbed and well rubbed in (this may take about 5 minutes, depending on area covering).
- Once you have applied a thin, well-rubbed-in layer of ointment onto the affected areas, you may notice that these areas end up feeling dry again. IMMEDIATELY, while the skin is still partially moist, rub another smidgin of ointment over the same spots of scaly skin. Rub in thoroughly once again. Follow this procedure at least twice a day for best results. For severe psoriasis you can repeat this process up to five times a day for maximum relief. When symptoms improve you can reduce this routine to once a day.
- For accelerated results, use natural sunlight therapy daily after one of your ointment applications: ten minutes of sunshine daily, after wetting and moisturising the skin as described. After short sun exposure don’t wash off the ointment by having a shower. Instead, if it’s necessary, you can gently blot any excess ointment with a wet cloth.
- TIP: Don’t try to remove dry patches of skin unless they are first wetted with water.
- There is little or no benefit to putting a cream or oil onto the skin unless the skin is moist.15
Ointment
Ointments and balms are thick and greasy. Look for beneficial ingredients such as pawpaw, triglyceride wax, and vitamin E. While not a cure, ointments can protect your skin from stinging when you go for a swim in the ocean or a chlorinated pool if a thick coat is applied beforehand. However, ointments can also stain your clothes if not used sparingly. Natural ointments are available from health food shops. Natural pawpaw ointments that may be suitable for WOL Therapy include Brauer and Natralus Natural (check ingredients before purchase). Lucas have pawpaw ointment that contains some petrochemicals but it is also a suitable option.
Psoriasis facts
- Psoriasis affects more than 500,000 Australians
- 7.5 million Americans have psoriasis according to the country’s National
- Psoriasis Foundation
- 2% to 3% of the world’s population is affected by psoriasis (at the time this statistic was calculated it totaled approximately 125 million people!).
- Psoriasis is present in all racial groups but it is slightly more common in fair-skinned people.
- FYI: you’re less likely to get psoriasis if you live somewhere tropical and sunny.
Source: 1. Fischer, K., The Healthy Skin Diet, Exisle Publishing, 2008; Medem: 2. Medical Library, 2005, ‘News from the American Medical Association: smoking associated with the severity of psoriasis’; 3. Boreham, D.R, Gasmann, H.C. and Mitchel, R.E. 1995, ‘Water bath hyperthermia is a simple therapy for psoriasis and also stimulates skin tanning in response to sunlight’, International Journal of Hyperthermia, vol.11, no. 6, pp 745-54; 4. Staberg, B., et. al. 1987, ‘Abnormal vitamin D metabolism in patients with psoriasis’, Acta Dermato-Venereologica, vol. 67, no. 1.
To view everything on the Joliee Skin website, please visit our Site Map page.

 Nothing will be posted on your behalf.
Nothing will be posted on your behalf.

